
Hand herpes, also known as digital herpes simplex or herpetic whitlow, is a painful, tingling viral infection of the fingers and hands. It is transmitted through direct contact with infected skin. Herpetic whitlow is caused by the herpes simplex virus (HSV). There are two types of herpes simplex virus. The first type, type 1 or HSV-1 affects the oral mucosa including areas of the mouth, nose, and face. The second type is HSV-2 which is an infection most often found around the genitalia and buttocks.
As herpetic simplex virus is highly contagious. It may infect other areas of the body including the skin of the hand, particularly around the fingertips and nail bed. Areas that are susceptible to infection are places of injury, broken skin, or a tear at the cuticle at the base of the fingernail. These areas can become inoculated with the infection through direct physical contact. It is most often transmitted during childhood. Also, practitioners who may work with infected patients, such as oral hygienists are susceptible as they may come into direct contact with infected oral mucosa.
Infected areas of the fingers and hands may experience pain, redness, or erythema, as well as swelling. These areas may develop into blisters. An infection of the hands or fingers may become noticeable within 2 to 20 days of exposure to a contagious sore of either HSV-1 or HSV-2. As the presentation of herpetic whitlow is similar to other issues which may be present in the fingers and hands, such as paronychia, simple calluses, seborrheic keratitis, and even squamous cell carcinoma, definitive diagnosis is important.
A hand herpes infection may be either primary or recurrent. A primary infection is the result of direct contact with either type 1 or type 2 of the highly contagious herpes simplex virus. Once a primary infection occurs, the virus remains in the body, becoming latent or hibernating in nerve cells. An infection may become recurrent due to certain triggers. Symptoms of a recurrent infection are often milder. These may occur in a similar area to the originating primary infection.
Hand Herpes or Herpetic Whitlow; Signs and Symptoms
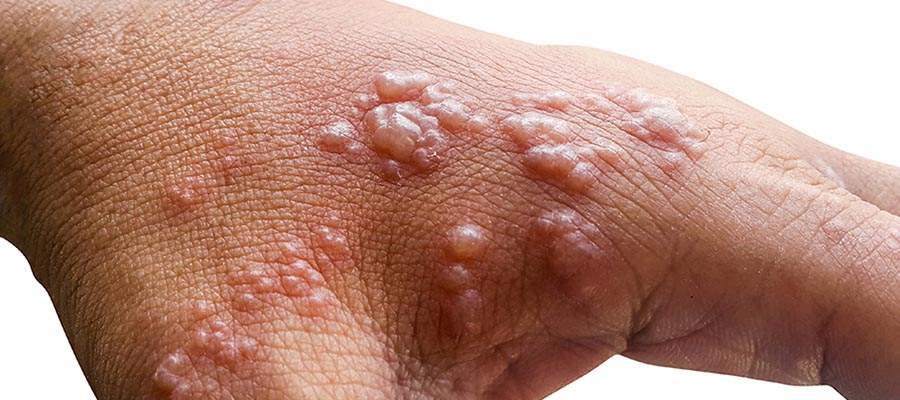
The appearance of Hand Herpes
Signs of hand herpes may begin 2 to 20 days after direct contact to skin infected with a herpes simplex virus. These signs may commonly be found on the thumb and forefinger, other fingers, and on other parts of the hand. Initially, the area of the finger becomes swollen and red. This is followed by small 1 to 3 mm fluid-filled vesicles or blisters. These may be clustered together above a bright red base. Over time, the blisters may burst leaving small depressions or lesions. These scab over and usually completely heal without leaving a scar.
Hand Herpes Symptoms
The swollen, red areas are often accompanied with burning pain and tingling. Other symptoms which may be associated with herpetic whitlow are fever, swollen lymph nodes in the elbow or underarm areas. At the site of infection, there may also be lymphangitis which appears as red streaks radiating from the infected area.
Herpetic whitlow is caused by broken skin which is exposed to the herpes simplex virus. Potentially, people with a history of genital herpes or cold sores may inoculate themselves with the infection in their own fingers and hands. It may also occur from direct contact with skin of other people infected with HSV-1 or HSV-2. As herpetic whitlow may be dormant in a patient who previously had a primary infection, recurrence is possible.
What Causes Herpetic Whitlow
Hand herpes or herpetic whitlow can be transferred from person to person by coming into direct contact with the herpes simplex virus, HSV-1 or HSV-2. Additionally, a person with HSV-1 or HSV-2 can develop herpetic whitlow as a secondary infection of the hand or fingers.
An open wound, injury, cut, or broken skin on the hand or fingers is the entry point for a primary or secondary infection.
Once an infection occurs, there is a potential for recurrence. The virus can become latent, and reactivation can occur months or even years after the initial presentation. Triggers which may exacerbate a recurrent infection are fever, illness, stress, trauma, and hormonal changes.
Who is Susceptible to Herpetic Whitlow?
Herpetic whitlow may affect people of any age, gender, or race. It is a rare infection with an incidence rate of 2.4 cases in 100,000 people per year.
Healthcare practitioners that are not able to wear gloves when being in contact with a patients’ oral mucosa are susceptible. Most notably, medical professionals who work as respiratory therapists or dental hygienists are at risk. They may contract herpetic whitlow through exposure to contagious lesions of patients infected with herpes simplex viruses.
Children who suck their thumbs or fingers can contract herpetic whitlow if they also have cold sores or herpes infection of the lips or mouth.
Activities That May Contribute to Hand Herpes
Sharing hygiene items such as towels, face cloths, and lip balm with others in the presence of an HSV infection may contribute to spreading the virus. Touching sores, even when applying medication, can also spread the virus. Always wash your hands and hygiene items. When possible, keep sores bandaged to limit exposure.

Differential Diagnosis – Is It a Viral Wart, or Something Else?
Seborrhoeic Keratosis
A common sign of aging skin, seborrhoeic keratosis are very common as we age. Over 90% of people aged 60 or over have some of these harmless warty spots. They often begin in people at age 30 to 40 and may occur in people of all genders and races.
They look like a papule or plaque and may range in size from a millimetre to several centimetres. These lesions are highly variable in appearance and can be found anywhere on the skin. They may be raised or flat. The surface might be smooth, waxy, or warty. They may appear in a broad range of colours from yellow, light brown, grey, dark brown, or black. Seborrhoeic keratosis can also be a mix of colours and found in groups or as solitary spots.
A seborrhoeic keratosis on the hand may be confused with other dermatological issues such as hand herpes. They may also appear as other skin issues which can be dangerous such as certain types of skin cancers, squamous cell carcinoma, and melanoma. For this reason, definitive diagnosis is appropriate in situations of seborrhoeic keratosis.
Calluses
A callus is an area on your hands, fingers, palms, toes, or soles of your feet that become hard and thick due to repeated friction. They are a natural reaction built in to protect skin from overwear. These areas can become sensitive or painful because of the excessive use. Often calluses will go away once the activity has changed or has stopped.
Paronychia
Paronychia is an infection around the skin of fingernails and toenails. Herpetic whitlow is often mistaken for paronychia. It is caused by a localised bacterial or yeast infection or abscess in the nail fold. Paronychia may have a sudden onset. It may also arrive slowly. The infection may resolve quickly within a day or two or last for several weeks. Paronychia is easily treated but can become severe if left untreated. Untreated paronychia may result in loss of part or total loss of the nail.
Squamous Cell Carcinoma
Squamous cell carcinoma (SCC) of the nail bed, or subungual SCC is rare, but it is the most common malignancy of the fingernail. Diagnosing SCC is challenging as the presentation is often similar to other nail disorders such as fungal infections, cystic lesions, and herpetic whitlow. Unfortunately, this challenging diagnosis may result in a delay in treatment. Treating subungual SCC may include a surgical approach which can preserve function. For this reason, excluding subungual SCC from the differential diagnosis is important when examining for herpetic whitlow.
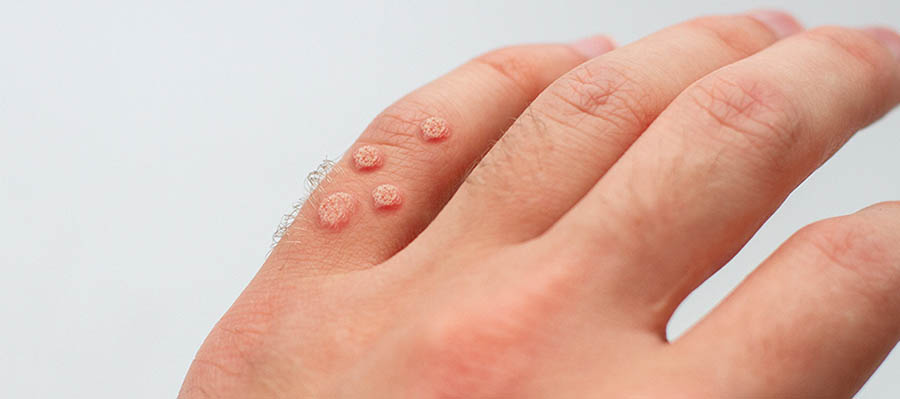
When to See a Doctor
Patients should visit a doctor if they notice a tender sore on the finger that does not go away. Importantly, seek medical attention if the tender, painful wart is accompanied by other symptoms typical of oral or genital herpes, or there has been recent contact with a known infection.
Specialised Treatment At CHARMS
At CHARMS, the specialist hand doctor will assess and definitively diagnose the viral infection. To lessen the severity and duration of symptoms, medication may be prescribed. Definitive diagnosis and treatment may also help to minimize the spread of infection.
What Are the Risks of Not Diagnosing Hand Herpes?
If left unattended, hand herpes is highly contagious. The infection may continue to spread to other parts of the body. Herpes Simplex Virus can also infect the eye. This is particularly important for contact lens wearers. Notably, the viral infection can also spread to family members and co-workers.
Minimising Herpetic Whitlow Discomfort Through Self-Care
Hand herpes can be painful with discomfort of burning and tingling sensations. It may also be combined with fever and pressure from swelling.
Take oral medications such as acetaminophen or ibuprofen to reduce pain and fever.
Apply a cool compress or an ice pack to relieve swelling and discomfort.
Keep the area clean and dry. Wash hands regularly. Try not to burst the liquid-filled blisters, as it may exacerbate the condition.
Helpful Lifestyle and Hygiene Practices to Decrease Contagious Spread of Hand Herpes
Avoiding infection and managing contagious infected areas are the best ways to prevent the spread of herpes simplex virus.
Wear gloves.
Particularly important for healthcare professionals who may be exposed to infected skin.
Bandage affected area of infection.
Keeping an area infected with herpes simplex virus clean and dry may help the area to heal. Provide a bandage to decrease the incidence of contagious spread.
Maintain a healthy lifestyle.
Maintaining a healthy lifestyle with good nutrition and low stress may reduce recurrent outbreaks of hand herpes.
Avoid sharing personal hygiene items.
Personal hygiene items such as hand towels and face clothes should be washed regularly. Anyone with an ongoing infection should keep their towels separate from others who may use them.

Conclusion: Treat Tender, Tingling Fingertips to Minimize Symptoms and Decrease Infection
Avoiding infection is the best defence against herpetic whitlow. Currently, there is no cure and recurrent infections are possible since the virus may remain dormant for years.
Definitive diagnosis and appropriate treatment are ways to minimise the spread of hand herpes. Using gloves and bandages in addition to keeping an area of infection clean and dry may help reduce the spread of the highly infectious herpes simplex virus. Maintaining a healthy lifestyle may minimise the duration of infection and rate of recurrence.